Healthcare organizations are generating an unprecedented volume of data. Electronic health records (EHRs), high-resolution medical imaging, and continuous remote monitoring feeds from wearables all contribute to an explosive growth in data. In fact, roughly 30% of all data generated worldwide is from healthcare settings, and an estimated 80% of healthcare data is unstructured content like medical images, PDFs, and free-text clinical notes.
Storing and managing this deluge is costly and complex: infrastructure expenses climb as data volumes soar, and strict compliance requirements (e.g., HIPAA, GDPR) add layers of security and auditing overhead. To make matters worse, data often lives in silos across legacy hospital systems, making integration and analysis difficult. The goal of this article is to examine modern healthcare data storage challenges and outline secure, scalable solutions to overcome them.
For healthcare executives and technical architects, the stakes are high. You need to keep medical data storage reliable and instantly accessible to clinicians, but also locked down to meet privacy laws. You must bridge aging on-premises systems with cloud services and break down silos so data flows where it’s needed.
We’ll explore why data storage in healthcare is harder than it looks, the technical requirements for HIPAA-compliant healthcare storage, and proven strategies for building scalable, multi-tenant architectures. Throughout, we’ll highlight how a modular backend approach (such as Edenlab’s FHIR®-centric Kodjin platform) can simplify health data storage management. By the end, you’ll have a clear roadmap to tackle modern healthcare data storage challenges head-on.
Why Healthcare Data Storage Is Harder Than It Looks
Storing data might sound as simple as buying bigger servers or more cloud space, but data storage for healthcare presents unique challenges that aren’t obvious at first glance. Healthcare data isn’t uniform; it spans numerous data types.
Structured records in databases (patient demographics, lab results) coexist with huge unstructured files like radiology imaging, ECG waveforms, and genomics data. This variety means healthcare data storage and retrieval must handle both transactional queries (e.g., fetching a medication list) and streaming gigabyte-sized images or sensor data. Traditional universal storage systems struggle under such diverse workloads.
Another obstacle is regulations. Laws such as HIPAA in the United States and GDPR in Europe aim to safeguard healthcare data, which is considered among the most sensitive types of information. Strict controls on access, privacy, and auditing are mandated under these standards.
There needs to be thorough planning before a hospital can simply upload data to the cloud; there needs to be encryption, access logs, patient consent management, and more. The problem is made worse by the widespread use of legacy systems in healthcare.
Even today, a large number of medical facilities are using PACS imaging systems and electronic health record platforms that are several decades old. Data is siloed in departmental systems since these older systems don’t have current APIs or aren’t scalable. Data integration or healthcare data migration from older storage systems to newer ones is not an easy or risk-free task.
Data exchange across systems is challenging due to the disjointed patchwork of old systems and different data standards; storing data centrally is an even bigger challenge. There are “considerable obstacles in attaining smooth, scalable, and dependable data exchange” when it comes to healthcare information exchanges (HIEs) that try to share data due to “a fragmented network of outdated systems” and uneven standards. That is to say, healthcare data storage solutions face interoperability challenges side by side with scale.
Technical Storage Requirements for Compliance and Scale
Overcoming these challenges requires a robust technical approach. Below are key requirements any modern secure data storage in healthcare system should meet to be both compliant and scalable:
- End-to-End Encryption: All sensitive health data should be encrypted both at rest and in transit. This means using strong encryption algorithms for stored files/databases and enforcing HTTPS/TLS for data transfer. Encryption ensures that even if infrastructure is compromised, the data remains unintelligible to unauthorized parties—a core need for healthcare storage compliance under regulations like HIPAA.
- Data Lifecycle Management: Effective health data storage management entails defining how long different data types must be retained and when they should be archived or deleted. For example, raw device telemetry might be retained for a shorter period than medical images required by law to be kept for years. Automated lifecycle policies (tiering older data to cheaper storage, purging expired records) help control costs while staying compliant with record-keeping rules.
- Redundancy and Disaster Recovery: Healthcare systems demand near-100% availability—clinicians need data 24/7. Thus, storage must have built-in redundancy: backups, replication across data centers or cloud regions, and failover mechanisms. A robust healthcare data storage solution will replicate data in real-time and perform regular backups so that no single point of failure (disk crash, network outage, etc.) can disrupt access or cause data loss.
- Tenant and Record Isolation: In multi-tenant or multi-department architectures, record isolation is crucial. Each clinic or client’s records should be logically (and often physically) isolated from others’. This can be achieved through separate databases or schemas per tenant, strict access controls, and data partitioning. On a per-user level, role-based access control (RBAC) ensures that staff only see the patient data they’re authorized to see. Isolation and RBAC together prevent data leakage between tenants or unauthorized access within an organization—essential for secure data storage in healthcare environments.
- FHIR® Compatibility and Interoperability: Modern healthcare storage should support interoperability standards like HL7® FHIR®. Storing clinical data in (or mapping it to) FHIR format enables seamless exchange via APIs and ensures that when data is retrieved, it’s already structured in a standard schema. Even if data isn’t stored natively as FHIR resources, having a FHIR healthcare data storage and retrieval layer (e.g., a FHIR server interface) greatly simplifies integration with other systems and third-party apps. Compatibility with DICOM for images and other relevant standards is also important.
- Auditability: Compliance demands audit trails. Every access or modification to stored medical data should be logged with who, when, and what was done. Robust audit logging and monitoring allow detection of any unauthorized access and are often legally required. In the event of a breach or an investigation, audit logs provide accountability. A scalable storage system will have centralized logging and tools to quickly produce reports for compliance audits.
Average healthcare breach cost: $9.77M (2024). Security controls in storage (encryption, access control, auditing, DR) are not optional overhead; they’re core architecture.
The above statistic underscores why these technical safeguards are non-negotiable. A single lapse in security or compliance can cost an organization tens of millions and, more importantly, erode patient trust. By investing in the measures listed—encryption, access control, redundancy, standardization, and auditing – healthcare providers build a foundation that protects them from both catastrophic data loss and regulatory penalties. Compliance at scale is achievable, but it must be engineered from the ground up.
Build encryption, access controls, audit logging, and privacy controls into your storage layer
to meet HIPAA/GDPR and reduce breach exposure. Check our
Health data security & privacy services
Building Scalable and Compliant Storage in Multi-Tenant Environments

Many healthcare software providers and hospital networks today operate in multi-tenant environments: for example, a Software-as-a-Service EHR platform serving multiple hospitals on one cloud infrastructure. Multi-tenancy introduces its own complexities for data storage. Here’s how to address them:
- Strong Tenant Isolation: As mentioned, each tenant’s data should be walled off. The storage design might give each client a dedicated database instance or use tenant-specific encryption keys so that even at the storage level, data sets don’t commingle. Isolation extends to backups and disaster recovery; one tenant’s backup should be logically separate from others’. This design ensures that a query or user from Hospital A can never access Hospital B’s records, a critical aspect of data storage for healthcare providers offering cloud services.
- Granular Access Control (RBAC): Within each tenant, implement Role-Based Access Control tied into your storage authorization. For example, an enterprise architecture may use a FHIR server with a SMART on FHIR authorization layer or custom RBAC rules so that only oncologists can retrieve oncology records, only patients can access their own data, etc. Granular permissions combined with robust authentication (single sign-on, MFA) maintain compliance in a user-friendly way.
- Automated Compliance Enforcement: Multi-tenant architectures should bake in compliance checks. This can include automatic encryption of any new data added, validation of data formats against standards (to ensure no sensitive info is stored in the wrong field), and continuous monitoring for anomalies. If your platform is deployed across regions, it should adhere to data residency laws (e.g., patient data from EU stays in EU data centers). Healthcare storage compliance can be maintained by using infrastructure-as-code and policy-as-code tools that enforce these rules uniformly across all tenants.
- Unstructured Data Management: A major challenge in multi-tenant health platforms is handling unstructured medical data storage (like imaging and documents) for each tenant at scale. Best practice is to use scalable object storage (cloud-based or on-premises) that can handle millions of large files, paired with a metadata index in a database. Store files in a structured path by tenant and patient ID, and use content-addressable storage or checksums to avoid duplicates. Also consider content management features: for example, auto-tag images with patient and study info for easy retrieval. By centralizing unstructured blobs in a secure, redundant store and linking them to patient records via metadata, you ensure that cloud-based healthcare storage of bulky data is efficient and compliant.
- Leverage Cloud Smartly: It’s no surprise that cloud platforms are popular for multi-tenant healthcare apps: cloud data storage in healthcare offers on-demand scalability, global availability, and managed security features. In fact, about 70% of healthcare businesses have now embraced cloud computing in some form. A cloud storage in healthcare approach can drastically cut infrastructure management efforts. However, when utilizing cloud services, choose those with healthcare compliance certifications (such as AWS or Azure with HIPAA-compliant configurations) and use built-in tools like AWS KMS or Azure Key Vault for managing encryption keys. Architect your cloud storage with a hybrid mindset: keep an option to deploy on private cloud or on-premises for clients that require it. This flexibility to go hybrid ensures even highly regulated providers can use your solution.
By following the above practices, you can build a multi-tenant storage architecture that scales to hundreds of facilities and millions of records while still treating each dataset with the care it deserves.
Think of it as a “private vault” for each tenant within a larger bank; the overall system is unified and efficient, but each customer’s valuables are locked away separately. With proper design, multi-tenancy does not have to mean sacrificing security or compliance. It is entirely possible to achieve both multi-tenant efficiency and per-tenant data privacy, as long as isolation and security controls are front-and-center in the design.
Conclusion
Modern healthcare organizations cannot afford to treat data storage as an afterthought. The combination of massive data growth, stringent regulations, and legacy integration issues makes health data storage one of the most critical challenges in healthcare IT today.
In this article, we discussed why storing health data is inherently complex, from the diversity in healthcare data storage methods needed (databases, object stores, etc.) to the compliance burdens every step of the way. We outlined the technical must-haves for a HIPAA-compliant healthcare storage solution, including encryption, redundancy, and audit trails, and how to design for multi-tenant scale with tenant isolation and standardized APIs.
The good news is that these challenges are solvable. By adopting a secure-by-design, modular architecture (for example, Edenlab’s Kodjin platform), healthcare providers and software vendors can turn storage from a pain point into a competitive strength.
Our experience shows that with proper planning, it’s possible to implement secure, scalable, and compliant storage solutions that integrate seamlessly with both modern and legacy systems. Whether you’re dealing with a sprawling hospital network or a healthtech startup platform, the key is to build in security and interoperability from day one.

In summary, tackling healthcare data storage challenges requires a blend of the right technology and expertise. With the strategies detailed above, healthcare CIOs and CTOs can ensure their data is not only safe and compliant but also readily available to drive better patient outcomes and innovation. Now is the time to break down those silos, modernize your storage infrastructure, and embrace the benefits of cloud and modular design, all while keeping patient data privacy sacrosanct.

Want an expert review of your healthcare storage architecture?
We’ll assess your current setup, identify risk hotspots, and propose a roadmap to modernize safely.
FAQs
What are the top healthcare data storage challenges today?
The biggest healthcare data storage challenges include managing the immense volume and diversity of data—from structured EHRs to unstructured imaging and notes—while maintaining compliance with regulations like HIPAA. Legacy systems create data silos that limit integration, and escalating storage costs demand smarter tiering and lifecycle management to avoid overspending.
What are the benefits of cloud storage in healthcare?
The benefits of cloud storage in healthcare include rapid scalability, high availability through geo-redundancy, and reduced IT burden, as infrastructure is managed by the provider. A cloud-based healthcare storage approach supports easy data sharing across organizations but must be configured to meet compliance with encryption, access controls, and BAAs.
How can we ensure secure data storage and retrieval in healthcare systems?
Ensuring secure data storage in healthcare involves encrypting data at rest and in transit, applying RBAC to restrict access, and maintaining audit logs to track activity. Data validation at retrieval (especially when using FHIR) ensures integrity, so only authorized users can access accurate and untampered health information.
What is HIPAA-compliant healthcare storage, and what features does it require?
HIPAA-compliant healthcare storage includes encryption, access controls, audit trails, data integrity checks, and robust backup/disaster recovery plans. It ensures ePHI is securely stored and monitored, often using certified cloud providers with signed BAAs and strong technical safeguards in place.
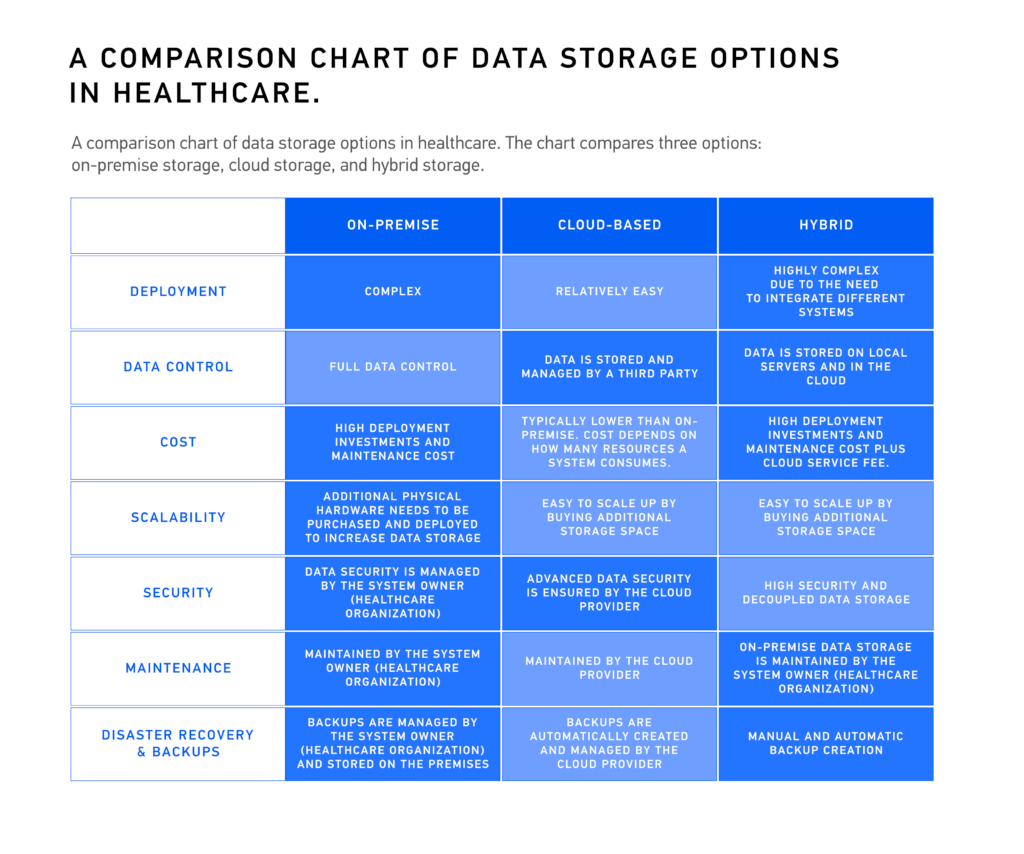
What healthcare data storage methods are commonly used (on-premises vs. cloud vs. hybrid)?
Common healthcare data storage methods include on-premises systems for control, cloud storage for scalability, and hybrid models combining both. Many also use co-location or private clouds. While no one method fits all, cloud data storage in healthcare is growing rapidly for its flexibility, especially when designed for compliance.
How can healthcare providers future-proof their data storage strategies?
To future-proof data storage for healthcare providers, focus on scalability, standards compatibility (e.g., FHIR), strong governance, and automation. Hybrid or multi-cloud readiness is key for flexibility. These steps ensure your health data storage architecture evolves securely with regulatory and technical shifts.
Stay in touch
Subscribe to get insights from FHIR experts, new case studies, articles and announcements
Great!
Our team we’ll be glad to share our expertise with you via email










