Interoperability in healthcare remains a big challenge for medium-sized organizations across the sector. Whether you’re a health payer processing claims, a provider managing patient records, or a pharmacy handling prescriptions, seamless data exchange is key.
Yet, many organizations still struggle with significant interoperability issues in healthcare. Remarkably, 35% of physicians rely only on fax, mail, or e-fax to exchange PHI. These legacy systems lead to inefficiencies, mistakes, and inadequate patient care that highlights ongoing problems with interoperability in healthcare. In short, we cover interoperability in healthcare benefits, challenges, and resolutions.
Today, interoperability often refers to moving toward a common data standard, specifically FHIR. If all organizations used this format, it would create an ideal scenario, supported by regulators and governments. However, the reality is different.
Interoperability involves helping organizations exchange data smoothly and digitally, while also allowing the data to be transformed and stored in their proprietary formats. It goes beyond mere integration — it focuses on maintaining data quality and meeting the specific standards of each organization.
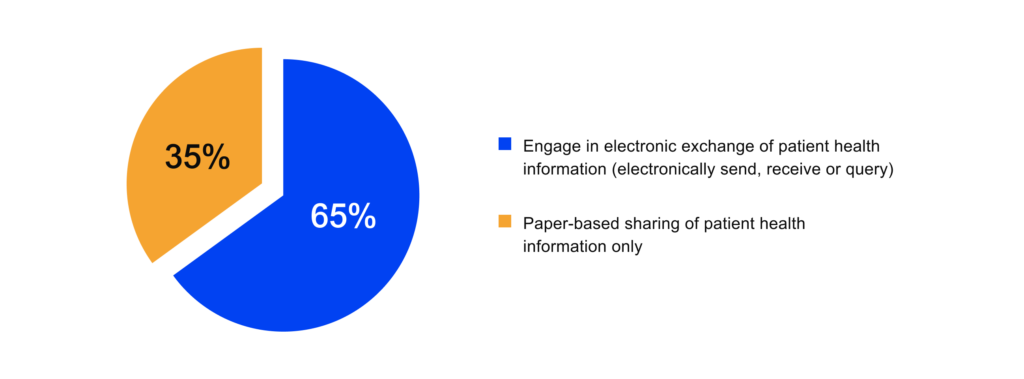
Description: Patient information exchange methods
This article explores proven approaches to handling the healthcare interoperability challenges. We’ll analyze the latest technological solutions transforming healthcare data exchange, examine real-world case studies, and deliver actionable recommendations to help you navigate interoperability in healthcare.
Highlights:
- Up to 26.9% of hospital data errors occur due to interoperability issues.
- Healthcare organizations can lose up to $20 million annually from inefficient data exchange.
- About 20% of patients may have incorrect medical records, risking patient safety.
- Over 90% of healthcare leaders plan to invest in new software to improve data management and interoperability.
The Cost of Inefficient Data Exchange in Healthcare & What To Do
Poor data exchange is costing money and harming patient care. Healthcare leaders report financial losses due to ineffective data use, with errors occurring in up to 26.9% of hospital data. These errors result in redundant tests, wrong diagnoses, and prolonged hospitalizations, driving annual losses to $20 million.
As we move into 2025, the focus on health data interoperability will be sharper than ever. Continued spread of value-based care models, technology-enabled innovation, and the combination of market-driven adoption with regulatory pressures drive the demand for smooth, high quality, interoperable data exchange across the health ecosystem.
Daniel Vreeman, Chief Standards Development Officer at HL7 International
The problem is complex. Many organizations rely on 20+ different software systems, this lack of interoperability creates silos and raises patient-safety risks. About 20% of patients may have incorrect medical records, risking their safety.
Addressing these challenges requires not only interoperability standards like FHIR, but also practical healthcare software integration that connects disparate platforms into a unified data ecosystem.

Description: Interoperability network
Healthcare executives are taking decisive steps to tackle healthcare interoperability problems. Over 90% invest in advanced solutions to reduce workforce burnout and enhance data operations. Many are focusing on tools to streamline workflows and use data more effectively, showing efforts on how to improve interoperability in healthcare.
Understanding Main Interoperability Levels
Healthcare experts typically identify several distinct levels of healthcare interoperability. Some of them can be achieved with current healthcare IT systems. Others will need innovations in patient-centered technology. Each layer builds upon the previous, offering more complex services, data exchange, and interpretation capabilities. They include:

Description: Main interoperability levels
- Foundational. This level involves secure data transfer between systems without interpretation. A nurse might download a patient’s lab results as a PDF and manually enter the data into the health record.
- Structural. Data follows a standard format for interpretation by many systems. Standards such as FHIR and HL7 create consistent records that can be moved easily between systems.
- Semantic. This level allows data exchange between systems with different structures. It aims to understand and process data regardless of its original format. For example, one healthcare system uses “patient ID” as a data field while another uses “patient record number”. In this case, semantic interoperability ensures that both systems recognize these terms as referring to the same concept. Complete implementation may require AI to comprehend the data’s context and significance.
“In 2025, healthcare organizations will move beyond standard data exchange to handle the more complex challenge of semantic interoperability — ensuring that clinical information is not just shared but meaningfully understood across systems and care settings.”
David Lareau, CEO of Medicomp Systems
- Organizational. This involves smooth data exchange between organizations with different rules and goals. Policy and technology innovations are required to ensure secure, integrated workflows across various groups. For example, hospitals and health insurance companies may have distinct policies that complicate sharing data. To address this, organizations need common data-sharing agreements and technology that support integrated workflows. For instance, an EHR system may need to adapt to meet the hospital’s and the insurance provider’s requirements.
Unlock the full potential of data exchange
Edenlab brings deep FHIR expertise, which is proven in large-scale implementations. We enable seamless integrations, advanced data modeling, and custom APIs tailored to your needs to help you discover the full potential of healthcare interoperability.
Learn moreThe Challenges of Healthcare Data Exchange: What’s Holding You Back?
Healthcare data exchange faces some challenges of interoperability that make sharing information tough. Each point below targets a core interoperability issue you can track and fix.

Description: Main interoperability challenges
Different Data Formats and Terminologies
Healthcare systems use various ways to code and communicate data. This lack of standard formats can cause errors when information moves between systems. It’s also challenging to combine data from different resources. For example, one system might label a diagnosis as “High Blood Pressure,” while another uses “BP” or employs proprietary codes rather than standardized terminology. Such differences disrupt workflows and impact patient care without proper mapping and transformation.
Outdated Standards
Legacy HL7 standards such as v2.x and v3 have been the cornerstone of healthcare data exchange for years. These traditional protocols, however, fall short of meeting contemporary healthcare’s sophisticated requirements. This gap drives the sector to explore a more advanced alternative — FHIR. This standard addresses many of the shortcomings of older ones. It offers better flexibility, easier implementation, and stronger support for modern web technologies.
Nevertheless, you should understand that achieving interoperability extends beyond FHIR implementation. The healthcare landscape is diverse, and different standards serve various purposes. HL7 v2 is still widely used and effective for many existing healthcare systems.
Limited Compatibility Between EHRs
Seamless data exchange remains a critical concern regarding interoperability in healthcare challenges. Legacy EHR systems remain widespread because they were the standard when first adopted. However, these older systems have limited capabilities for true semantic interoperability, making data exchange less efficient. These limitations are common EHR interoperability challenges.
Organizational Readiness
Many hospitals and healthcare providers aren’t prepared to share data effectively. They may lack the right technology, trained staff, or management structures. These challenges with interoperability in healthcare impact how well an organization can share data.
Get inspired by our success stories
See how Edenlab’s FHIR expertise powers large-scale healthcare solutions. Check out real-world case studies. Look how advanced data integration, custom APIs, and scalable architectures make a difference.
Explore case studiesKey Interoperability Strategies
Organizations have two main approaches to address these interoperability problems in healthcare, and they don’t have to choose just one. The first step is joining existing networks to quickly enhance data exchange capabilities. At the same time, they can develop their connected ecosystem to maintain control over data flow and integration.
Another aspect to consider is establishing a single source of truth or relying on point-to-point integration. Both approaches offer unique advantages in addressing interoperability challenges in healthcare.
Joining Trusted Interoperability Ecosystem
This strategy connects to established health information exchanges (HIEs) and health information networks (HINs). It works well for smaller providers with limited resources that need to improve data sharing, meet regulations, and enhance patient care coordination.
| Pros: | Cons: |
| Faster implementation and time-to-value. Leverages established standards and protocols. Potentially lower initial costs. Access to a broader network of healthcare providers. | Less control over network governance and evolution. May require adapting to pre-existing standards that don’t fully align with organizational needs. Potential for vendor lock-in. |
Edenlab streamlines connectivity to established health exchanges, from CommonWell and Carequality in the US to eHDSI in the EU and various regional networks. Major EHR vendors like Epic also operate their HIEs, and for organizations seeking an alternative path, partnering with an EHR development company may provide more control over system architecture and integration strategy. Our integration process facilitates, validates, and optimizes collaborative workflows. This ensures smooth implementation across diverse healthcare ecosystems.
Building Your Connected System
This approach involves creating a custom interoperability solution tailored to an organization’s needs. It’s best for organizations with unique interoperability requirements not met by existing networks.
| Pros: | Cons: |
| Full control over network design and governance. Ability to tailor the network to specific business requirements. Potential for long-term cost savings. Greater flexibility in choosing technology partners. | Higher initial costs and resource requirements. Longer implementation time. Challenges in achieving critical mass for data exchange. Responsibility for ongoing maintenance and updates. |
Beyond connecting to existing networks, Edenlab helps organizations build their own HIE networks by engaging experienced HIE software developers. As integrations, data standardization, and normalization experts, we ensure seamless interoperability across all your subsidiaries and partner organizations. Whether interconnecting existing software or developing a localized HIE in healthcare, we streamline workflows, enhance data consistency, and reduce operational costs.
Single Source of Truth vs. Point-to-Point Integration
Building a connected system opens up new opportunities, yet challenges for interoperability in healthcare, especially when placing the semantic layer. The single source of truth and point-to-point integration models are two primary approaches to consider when implementing your healthcare interoperability solutions. Each has benefits and is suited to different business needs and tech settings.
Creating a Single Source of Truth
Creating a Single Source of Truth means building a centralized database to store healthcare data in a standardized format; many organizations now engage health data platforms development services to build this foundation for interoperability. This approach suits organizations with complex data management needs. It allows dynamic app connections and disconnections, optimizes coordination across clinic network branches, enables data analysis from multiple sources, and supports AI solution development.
This model provides a robust foundation for advanced healthcare analytics and seamless interoperability across diverse systems and applications by centralizing data in a standard format.
To put this into practice, organizations often rely on healthcare analytics product experts who can design, implement, and optimize solutions for real-world clinical and operational needs.
| Pros: | Cons: |
| Faster query responses due to pre-formatted FHIR data. Consistent data structure across the organization. Simplified data management and version control. Potential for advanced analytics on standardized data. | Requires significant capital costs in infrastructure. Introduces data duplication, which can lead to synchronization challenges. May require major changes to current systems and workflows. |
Point-to-Point Integration
The point-to-point integration model acts as a standardized interface layered over proprietary data systems, ensuring consistency in formats and terminologies across different healthcare solutions. Rather than storing data in an intermediate database, it dynamically translates and delivers information in the required format, making interoperability a seamless data transformation.
This model benefits organizations by enabling efficient data exchange and process digitalization, focusing on immediate needs rather than long-term strategic use of shared data. It allows them to achieve quick FHIR compliance and standardize interoperability health information exchange without completely overhauling their existing systems.
The point-to-point integration model is versatile. It makes this strategy a potent tool for solving challenges of interoperability in healthcare. The table below outlines its key benefits and drawbacks:
| Pros: | Cons: |
| Minimal disruption to existing systems and workflows. Lower initial implementation costs. Maintains a single source of truth in original systems. Easier to implement incrementally. | Potential for slower query responses due to real-time translation. May face challenges with complex data transformations. Requires ongoing maintenance of the translation layer. |
Edenlab team can implement both models. We create a robust database and server equipped with tools for ingesting, transforming, and normalizing data from various sources for the single source of truth approach.
In the point-to-point integration model, we handle on-the-fly transformation and standardization to ensure consistency and can create HL7 or FHIR interfaces to simplify the integration process.
The FHIR Facade solution is a similar approach, which allows organizations to maintain their existing systems while enabling seamless data exchange. Recently, we demonstrated the power of our FHIR Facade solution for a major Hong Kong healthcare company. Our team implemented the system in just four weeks without changing their current systems.
You can better understand the pros and cons of FHIR facade in our recent article.
Not sure which strategy is the best choice for your organization’s needs? Our healthcare technology consultants are here to help. We assess your current infrastructure, interoperability goals, and future scalability requirements. Through this tailored consultation process, we’ll recommend the optimal solution.
Actionable Strategies for Overcoming Interoperability Challenges
How to achieve interoperability in healthcare? Unfortunately, it’s a challenge without a quick fix. Moreover, it requires the collective actions of multiple stakeholders. Let’s explore some ways to improve interoperability in healthcare:
Standardize Data Exchange Protocols
Embrace the future of healthcare data sharing with FHIR. This standard enables seamless, real-time data exchange across diverse healthcare systems. By adopting FHIR, you’re not just keeping up but leading the way in efficient, standardized communication.
Modernize Legacy Systems
Embrace modern technology by transitioning to cloud-based platforms. This strategic move enhances integration capabilities and delivers exceptional flexibility. Cloud technologies enable adaptation to emerging demands and innovations that maintain your competitive advantage.
Prioritize Security
Implement robust identity verification and access control via authentication services. For FHIR platforms, adopt SMART on FHIR protocols to enable standardized security measures.
Build an Interoperable Ecosystem
Envision a healthcare ecosystem with flawless data integration across your enterprise and partner networks. Our solution delivers a robust, standards-based interoperability framework that connects your organization with HIE and healthcare networks. This strategic approach eliminates data fragmentation, maximizing operational performance and clinical outcomes.
Follow Data Exchange Regulations
Implement API-enabled, FHIR-native solutions for healthcare interoperability to meet various international standards and regulations. Ensure your API-driven, FHIR-native solutions align with HIE standards while meeting CMS, ONC, and regional certification requirements. For health payers in the USA, our solutions help meet CMS standards. In turn, healthcare providers, EHR vendors, and health IT developers can achieve compliance with ONC mandates. In Europe, we back the IPS, ISiK, and MedMij certification standards. We also support Germany’s telematics infrastructure requirements.
Edenlab is your reliable partner in achieving compliance with healthcare regulations and interoperability standards. We’ve recently worked with Elation Health to implement an FHIR-compliant solution that integrates ElationEMR platform with FHIR standard. Our Kodjin FHIR Server has helped Elation Health achieve ONC certification and improve data interoperability.
Looking for a Proven Solution?
At Edenlab, we’re revolutionizing healthcare interoperability with advanced solutions tailored to the unique needs of medical organizations. Our expertise includes:
- FHIR interoperability implementation
- Seamless legacy system integration
- Custom API development
- Data security and privacy
- HL7 FHIR services.
The Kodjin Data Platform, a robust foundation for healthcare data exchange, is at the core of our products. Kodjin delivers a powerful FHIR Server along with sophisticated data mapping tools and streamlined ELT processing. The platform integrates a comprehensive Terminology Service for code standardization and FHIR Analytics for data-driven intelligence.

Description: Components of Kodjin
Kodjin’s versatility suits HIEs, enterprise data fabrics, and SMART on FHIR apps. Its scalability has been proven in large-scale implementations, supporting up to 40 million users. We’ve connected 10,000+ healthcare providers to national HIE systems, proving our expertise in implementing solutions to interoperability.

Conclusion
Organizational interoperability in healthcare is more than a tech issue. It’s a must if you want to stay ahead of the competition. As you aim for smooth data exchange, you may face challenges with interoperability globally in healthcare. These include outdated standards, various data formats, and limited compatibility. Also, organizational readiness and other barriers to interoperability in healthcare.
The journey to clinical data interoperability is complex, but the rewards are substantial. Interoperability helps companies reduce data exchange time by adopting robust interoperability solutions in healthcare, potentially saving millions annually. They also get significant benefits in efficiency, patient care, and coordination.
At Edenlab, we lead the way in FHIR implementation, legacy system integration, and custom API development. We help thousands of healthcare providers gain seamless interoperability.
Want to transform your healthcare data exchange and pioneer interoperability excellence? Discover how Edenlab can build a tailored solution that positions your organization at the forefront of healthcare technology.

Break through healthcare interoperability barriers
From connecting legacy EHRs to building standards-based ecosystems, Edenlab helps medium-sized healthcare organizations achieve seamless data exchange. Whether you need quick wins with existing networks or a custom interoperability strategy, our expertise in FHIR and large-scale integrations ensures your systems work together securely.
FAQs
What is the role of FHIR in healthcare interoperability?
FHIR is a unified protocol allowing different healthcare platforms to interact seamlessly. It streamlines the transfer of PHI between EHRs, mobile apps, and different medical systems. FHIR also speeds up interoperability adoption, minimizing expenses and complications. This improved data sharing improves patient outcomes, as clinicians can retrieve PHI efficiently and safely.
How long does it take to implement an interoperability solution?
Deploying a healthcare data exchange system requires strategic planning. This way, project duration varies based on implementation scale. While comprehensive integration programs may take years, focused interoperability solutions can be executed more rapidly. We’ve successfully implemented FHIR facade solutions in about 4–6 weeks.
Who are the local stakeholders who might be involved in the challenge of interoperability?
Key local stakeholders in healthcare interoperability include healthcare providers like physicians and hospitals. They also count Regional HIEs, administrative bodies including Integrated Care Boards, Primary Care Networks, and decision-makers. Individual GP practices, community health centers, and local health departments also play vital roles.
How do custom software solutions help with healthcare interoperability?
Custom software solutions transform healthcare interoperability by addressing specific organizational challenges. We develop tailored solutions integrating with existing systems like EHRs, LIS, RIS, and PMS.
We execute system connections through DB-to-DB or flat file interfaces and standardized formats like CDA, FHIR, X12, XML, and JSON. Our healthcare interoperability experts can also develop or apply converters to transform data from one format to another.
Stay in touch
Subscribe to get insights from FHIR experts, new case studies, articles and announcements
Great!
Our team we’ll be glad to share our expertise with you via email










