Legacy HL7® interfaces (v2 and v3) power many hospital systems today, but they can be brittle, custom, and tough to scale. On the other hand, the HL7® FHIR® standard promises a more flexible, API-driven approach, but adopting it raises questions about compatibility with existing infrastructure and long-term support.
This article explains what HL7 and FHIR are in practical terms, and what the difference is between HL7 and FHIR for real-world projects. We’ll compare HL7 vs. FHIR head-to-head, including HL7 v2 vs. FHIR and HL7 v3 vs. FHIR, so that you can choose a future-proof path for your healthcare platform.
Drawing on Edenlab’s interoperability projects, we’ll share actionable advice. You’ll see how teams can layer FHIR on top of legacy systems to meet new interoperability demands without “ripping and replacing” everything. For example, Edenlab helped one EHR vendor avoid a full rewrite by implementing a FHIR facade, achieving compliance and real-time data exchange on top of a legacy HL7 data store.
Highlights:
- HL7 v2 is a decades-old messaging standard that was still running in 95% of U.S. healthcare organizations as of 2021, but its outdated design hinders scalability and requires heavy custom mapping.
- HL7 v3 introduced a formal data model (RIM) and XML format to improve consistency, but its complexity and lack of backward compatibility led to limited adoption; it’s now largely confined to niche projects (e.g., some Canadian systems).
- FHIR (Fast Healthcare Interoperability Resources) is the modern HL7 standard designed for real-world use: it’s API-driven, modular, and web-friendly. FHIR enables real-time data sharing and easier integration with mobile/web apps, aligning with government mandates for interoperability.
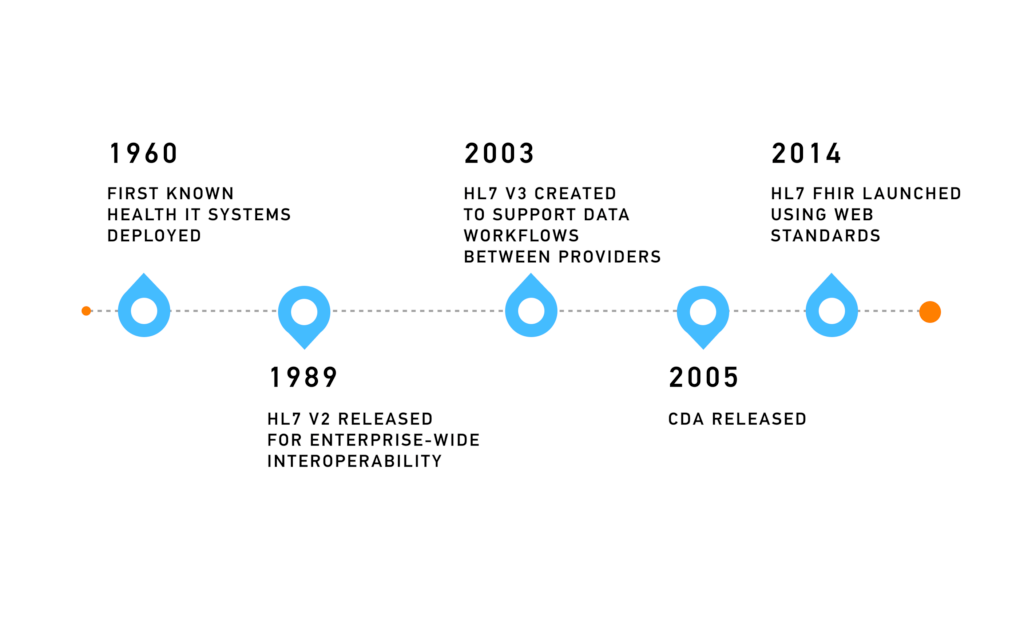
HL7 Version 2 (v2), first released in 1989, became the workhorse of healthcare data exchange. It’s a plaintext, pipe-delimited messaging standard that was revolutionary 40 years ago, allowing disparate systems to share basic information (admissions, lab results, billing events, etc.) in a common format.
Its success came from being simple and lightweight: HL7 v2 messages are just ASCII text segments with one-character delimiters. There’s no heavy computing or complex architecture needed; one system sends a text message, the other receives and parses it. This made HL7 v2 extremely effective for its era, when no real alternatives for electronic data exchange existed.

However, “legacy” is the keyword for HL7 v2. It was designed as a flexible framework, which ironically means every installation can be a bit different. There is no explicit data model or semantic framework built into HL7 v2 messages. Each interface defines its own segments and codes to some extent, so connecting two HL7 v2 systems often requires custom mapping logic.
Over time, hospitals have accumulated hundreds of such custom interfaces—fragile point-to-point links that are hard to maintain or extend. The format itself is also dated: a non-XML, non-JSON notation that’s challenging for non-experts to read and definitely not geared toward modern web or mobile applications.
HL7 Version 3 (v3) was HL7’s attempt in the mid-2000s to overcome v2’s limitations. If HL7 v2 was an 80/20 pragmatic solution, HL7 v3 in healthcare was meant to be a comprehensive, model-driven standard. It introduced the Reference Information Model (RIM) to rigorously define clinical data structures, and it used XML for encoding messages to be more precise and computer-readable.
Message example:
<observationEvent>
<id root="2.16.840.1.113883.19.1122.4" extension="1045813"
assigningAuthorityName="GHH LAB Filler Orders"/>
<code code="1554-5" codeSystemName="LN"
codeSystem="2.16.840.1.113883.6.1"
displayName="GLUCOSE^POST 12H CFST:MCNC:PT:SER/PLAS:QN"/>
<statusCode code="completed"/>
<effectiveTime value="200202150730"/>
<priorityCode code="R"/>
<confidentialityCode code="N"
codeSystem="2.16.840.1.113883.5.25"/>
<value xsi:type="PQ" value="182" unit="mg/dL"/>
<interpretationCode code="H"/>
<referenceRange>
<interpretationRange>
<value xsi:type="IVL_PQ">
<low value="70" unit="mg/dL"/>
<high value="105" unit="mg/dL"/>
</value>
<interpretationCode code="N"/>
</interpretationRange>
</referenceRange>
What happened in practice? HL7 v3 turned out to be too complex and not backward compatible with v2, so real-world adoption was minimal. Vendors were reluctant to rebuild their v2-based products from scratch for v3, especially since v3 messages couldn’t talk to v2 messages.
The standard’s steep learning curve and over-engineered design made implementations lengthy and costly. As a result, most healthcare providers and software companies skipped HL7 v3 entirely. Outside of specific government-driven projects (for example, Canada’s national EHR initiatives used some HL7 v3 standards), v3 never gained the ubiquity that v2 did.
So if you’re comparing HL7 or FHIR for a new project, most will agree that jumping from HL7 v2 to FHIR (and bypassing v3) is the logical move. In fact, many modern healthcare startups and projects choose FHIR from day one, both due to technological advantages and because regulators increasingly favor or even require FHIR.
(Need help integrating old and new standards? See our healthcare integration solutions for how we bridge HL7 v2 interfaces with modern FHIR APIs.)
FHIR: Designed for Real-World Use
Fast Healthcare Interoperability Resources (FHIR) is HL7’s modern standard for exchanging healthcare data, first released in 2014 and now widely regarded as the future of health IT interoperability. Unlike prior HL7 standards, FHIR was built by developers for developers with the realities of the web era in mind. Here’s what makes FHIR fundamentally different:
- API-First and Web-Friendly: FHIR uses a RESTful API approach over HTTP, similar to APIs in other industries. Data is accessed via standard URLs and exchanged in formats like JSON or XML. This means any team familiar with web development can work with FHIR—a much lower barrier than older HL7 specs.
- Modular “Resources”: FHIR breaks down health information into modular components called resources (Patient, Observation, Medication, etc.). Each resource has a defined structure and meaning. These are like LEGO blocks that can be assembled into more complex workflows. For example, a discharge summary can be a Bundle of Patient + Encounter + MedicationRequest + Observation resources.
- Flexibility and Extensibility: While FHIR resources have core definitions, they are designed to be extended for specific needs (through an extension mechanism) without breaking interoperability. There are also implementation guides and profiles (like U.S. Core, UK CareConnect, etc.) that tailor FHIR to regional requirements. The core standard is consistent, but you can adapt it as needed with a defined method.
- Multiple Exchange Paradigms: FHIR primarily emphasizes REST APIs, but it doesn’t ignore other modes. It also supports messaging (you can send a FHIR resource as a message payload) and documents (a Composition resource can serve a document similar to CDA). Thus, FHIR can coexist with older workflows and gradually replace them.
- Ease of Implementation and Testing: The FHIR community provides many tools: reference servers, validators, client libraries, etc. There’s an active ecosystem (including major EHR vendors like Epic and Cerner, which expose FHIR APIs, and big tech like Apple and Google, embracing FHIR for health data). The learning curve for basic FHIR use is far gentler than HL7 v3’s was. Developers can often get a basic FHIR interface working in days using open-source libraries, whereas implementing a new HL7 v2 interface or v3 interface from scratch could take weeks or months of painstaking mapping.
This agility means FHIR is production-ready in a very tangible sense: many hospitals and apps are already using it. In 2020, the U.S. CMS and ONC final rules formally required payers and providers to offer certain data via FHIR APIs, accelerating adoption.
Internationally, governments in Canada, Australia, the UK, and the EU are also backing FHIR for national health information exchange programs. Crucially, FHIR is also built to coexist with legacy systems, which is why teams debating “FHIR or HL7?” should recognize it’s not always an either/or: you can introduce FHIR incrementally alongside HL7 v2.
At Edenlab, we’ve made FHIR a cornerstone of our integration solutions. We’ve developed our own FHIR-based tools: the Kodjin Interoperability Suite. These tools help clients accelerate FHIR adoption by providing ready-made infrastructure.
We ensure that moving to FHIR doesn’t mean starting from scratch: we connect the dots between your HL7 and FHIR standards, mapping existing data to FHIR resources, and setting up the necessary modules (authentication, logging, etc.) so that your new FHIR APIs perform in a secure, production-grade way.

When to Migrate, When to Integrate
| Feature | HL7 V2 | HL7 V3 | FHIR |
| Overview | Widely used, older standard for data transmission between systems | Complex, highly structured data exchange standard | Modern data exchange standard with flexible elements and web-based approach |
| Data Format | text-pipe-and-hats messages | XML-based | JSON, XML, RDF |
| Interoperability | Limited, version-specific | Present but difficult to achieve | High, flexible |
| Implementation Complexity | Lower, due to simplicity | High, due to complexity | Lower, implementor-friendly |
| Flexibility | Low | Moderate | High, modular |
| Use Case | Admit discharge transfer patients, medical prescriptions, measurement results, etc. | CDA is the most commonly used component of the V3 standard (for clinical doc’s exchange) | Cover all common healthcare use cases. Used for exchange of such documents as a/b test results, clinical letters, scans, etc. |
| Adoption Rate | High in legacy | Very low | Rapidly growing |
| Resources (technology availability) | Work for exchange between systems within an organization and provides enterprise-level interoperability | Implementation of the common data model (RIM) is mandatory, making it too complex and unprofitable | Appeal to web-savvy developers but may require training costs and additional time or the help of certified FHIR experts |
From HL7 v2 feeds and custom mapping to production-grade FHIR APIs, we help teams design and implement interoperability that scales.
Check our
Healthcare Interoperability solution developmentDeciding FHIR vs. HL7 for your organization isn’t always a binary choice. In many cases, the right strategy is a blend: integrate FHIR gradually and migrate legacy interfaces over time. Here are some practical guidelines, drawn from our experience delivering healthcare integration projects:
Read also:
Read the case studyUse FHIR for New Capabilities
If you’re building new modules or exposing data to new consumers (patient apps, partner APIs, analytics dashboards), implement those interfaces in FHIR. This lets you meet modern interoperability needs out of the box.
This FHIR facade approach allows compliance with new regulations and integration with third-party apps without altering the core legacy system. In general, starting small with FHIR and expanding later is very feasible. You might begin with just patient and allergy data, then add more resource types as demand grows.
Maintain HL7 v2 for Internal/Legacy Processes
It’s often not realistic (or necessary) to replace every internal feed or device interface with FHIR overnight. Many hospital devices (lab analyzers, admission systems) still speak v2, and they work fine. Rewriting these could be costly and risky. Instead, continue to use HL7 v2 internally where it’s stable, and integrate by converting data to/from FHIR at the boundaries.
Modern interface engines or integration layers can map HL7 v2 messages to FHIR resources fairly seamlessly. Yes, there is effort in mapping, but it spares you from touching systems that aren’t ready for change. Over time, as those legacy systems age out or get upgrades, you can then migrate those endpoints to native FHIR.
Gradual Migration Plan
We recommend developing a roadmap where FHIR adoption is phased. Identify quick wins (like exposing a read-only FHIR API for key data), then medium-term goals (like replacing batch file transfers with FHIR subscriptions or messages).
Also consider where regulatory deadlines demand action. For example, if a government rule says all patient access must be via FHIR API by next year, that becomes a top priority (and a strong justification for the budget). Aligning interoperability upgrades with compliance timelines is smart. How do you align with compliance deadlines?
Start by mapping out upcoming requirements (US ONC Cures Act, EU EHDS, etc.) and use those as milestones in your FHIR migration plan. In our projects, we often conduct an interoperability audit to see which existing interfaces will be non-compliant or insufficient in one to two years, then target those for FHIR rollout first.
Cost and Scalability Considerations
Many ask about the long-term costs and support implications of sticking with HL7 v2 versus moving to FHIR. Legacy systems might seem cheaper now, but consider the opportunity cost: It’s getting harder to find engineers fluent in older HL7, and custom code for v2 can become a maintenance liability.
Moreover, staying on v2 could limit your growth: integrating with new partners (telehealth providers, national health info exchanges, etc.) often demands FHIR. On the flip side, adopting FHIR has an upfront cost (training, new development, possibly new FHIR server infrastructure), but it pays off in scalability. Choosing a standard isn’t just a tech decision; it shapes your product’s speed, scalability, and compliance. We advise clients to view FHIR adoption as an investment in agility: enabling quicker partnerships and innovations that might be impossible with the old stack.
With careful planning, you can ensure that you meet today’s needs with FHIR while keeping legacy systems running until you’re ready to decommission or upgrade them.
Conclusion: Interoperability That Works Today and Scales Tomorrow
Upgrading your interoperability standard is a strategic move that can future-proof your healthcare product. HL7 v2 gave us a long run of basic connectivity, but the future is being built on FHIR. The transition doesn’t happen overnight; it’s a journey of integrating standards, training your team, and refactoring interfaces.
But the end result is worth it: a more flexible architecture, the ability to plug into new healthcare ecosystems, and compliance with emerging regulations. By adopting FHIR (even gradually), organizations position themselves to deliver better patient and provider experiences through real-time data sharing, all while ensuring that they are aligned with the broader industry’s direction.
At Edenlab, our mission is to help healthcare companies achieve interoperability that works today and scales tomorrow. In practical terms, this means solutions that fit into your current environment (be it HL7 v2, v3, or a mix) and incrementally transform it for the better. Whether it’s building a FHIR API for a legacy EMR, mapping complex data to FHIR standards, or providing a fully managed FHIR platform, we have the expertise to make it a smooth process.
If you’re unsure how to proceed or want to accelerate this journey, Edenlab is here to help. From technical consultations to full-scale HL7/FHIR medical data migration projects, we partner with you to achieve interoperability that is not only standards-compliant but truly adds value to your product and users.

We dive deep where others skim
We’ll assess your current interfaces, define the right migration path (facade vs. repository), and help you roll out FHIR safely step by step.
FAQs
How can my current infrastructure support a shift to FHIR?
You don’t need to replace your HL7 v2/v3 systems to adopt FHIR. A common approach is a FHIR facade: you keep legacy feeds and databases as-is and add a FHIR API layer on top that maps existing data into FHIR resources. This gives you modern interoperability (apps, partners, compliance) without rewriting the core system.
Can we start small with FHIR and expand later?
Yes, and it’s often the best way. Start with a small set of high-value resources (e.g., Patient, Encounter, Observation, AllergyIntolerance) and a limited scope (read-only API, one integration). Once the patterns, mapping, security, and performance are proven, you can expand to more resources and workflows step by step.
How do I align interoperability upgrades with compliance deadlines?
Treat compliance dates as milestones in your roadmap. First, identify which regulations apply (e.g., patient access APIs, data export requirements), then map them to concrete deliverables like FHIR endpoints, OAuth security, audit logging, and export workflows. Prioritize the interfaces that must be compliant first, and phase the rest based on cost and impact.
What’s the business risk of staying on HL7 v2 or v3 too long?
The biggest risk is slower delivery and higher integration costs. Legacy HL7 environments tend to accumulate custom mappings, fragile point-to-point connections, and hard-to-maintain logic. Over time, this makes new partnerships, patient apps, analytics, and compliance updates more expensive and limits how fast you can scale or launch new capabilities.
What is the new HL7 standard that allows more interoperability?
HL7 FHIR (Fast Healthcare Interoperability Resources) is the modern HL7 standard designed for stronger interoperability. It’s API-driven, modular, and web-friendly, making it easier to integrate across systems and support real-time data exchange for modern healthcare ecosystems.
Stay in touch
Subscribe to get insights from FHIR experts, new case studies, articles and announcements
Great!
Our team we’ll be glad to share our expertise with you via email








