Every patient has a unique medical story, from genetics and family history to lifestyle and preferences. With such diversity, a versatile approach to care is outdated, often ineffective, and even needlessly costly. This realization is driving a shift toward personalized care, where treatment plans and preventive strategies are tailored to the individual.
However, delivering truly personalized healthcare at scale comes with challenges. It demands vast data integration, adherence to healthcare regulations, and significant clinical effort. Fortunately, advances in health IT—notably the HL7® FHIR ®(Fast Healthcare Interoperability Resources) standard and artificial intelligence (AI)—are emerging as key enablers.
Forward-thinking providers are transforming patient care with FHIR for personalized medicine and AI-driven automation to make individualized medicine practical and sustainable. In this article, we explore what personalized healthcare means, why it’s important, the hurdles it faces (from cost to time constraints), and how using FHIR to personalize healthcare data and AI-powered automation can help overcome these challenges.
Highlights
- Personalized healthcare improves outcomes by tailoring prevention, diagnostics, and treatment to each patient, but it increases short-term workload and costs.
- Healthcare systems traditionally rely on standardized protocols to cope with limited resources, yet this approach fails to account for individual differences.
- FHIR and AI-driven automation solve the key bottlenecks by integrating scattered data sources, reducing clinician burden, and enabling personalization at scale.
- Long-term, personalized care is more cost-effective but requires upfront investment, data interoperability, and the ability to aggregate information from EHRs, wearables, registries, and mobile apps.
What Is Personalized Healthcare?
Personalized healthcare is an approach to medicine that designs care around the individual patient rather than generic protocols. It is a proactive, patient-centered strategy that uses a person’s distinctive genetic profile, medical history, lifestyle factors, and even social determinants to create a tailored care plan. The goal is to catch diseases earlier, target interventions to patient-specific risks, and improve outcomes and quality of life. Instead of relying on statistical averages, personalized healthcare recognizes that each person’s health journey is unique.
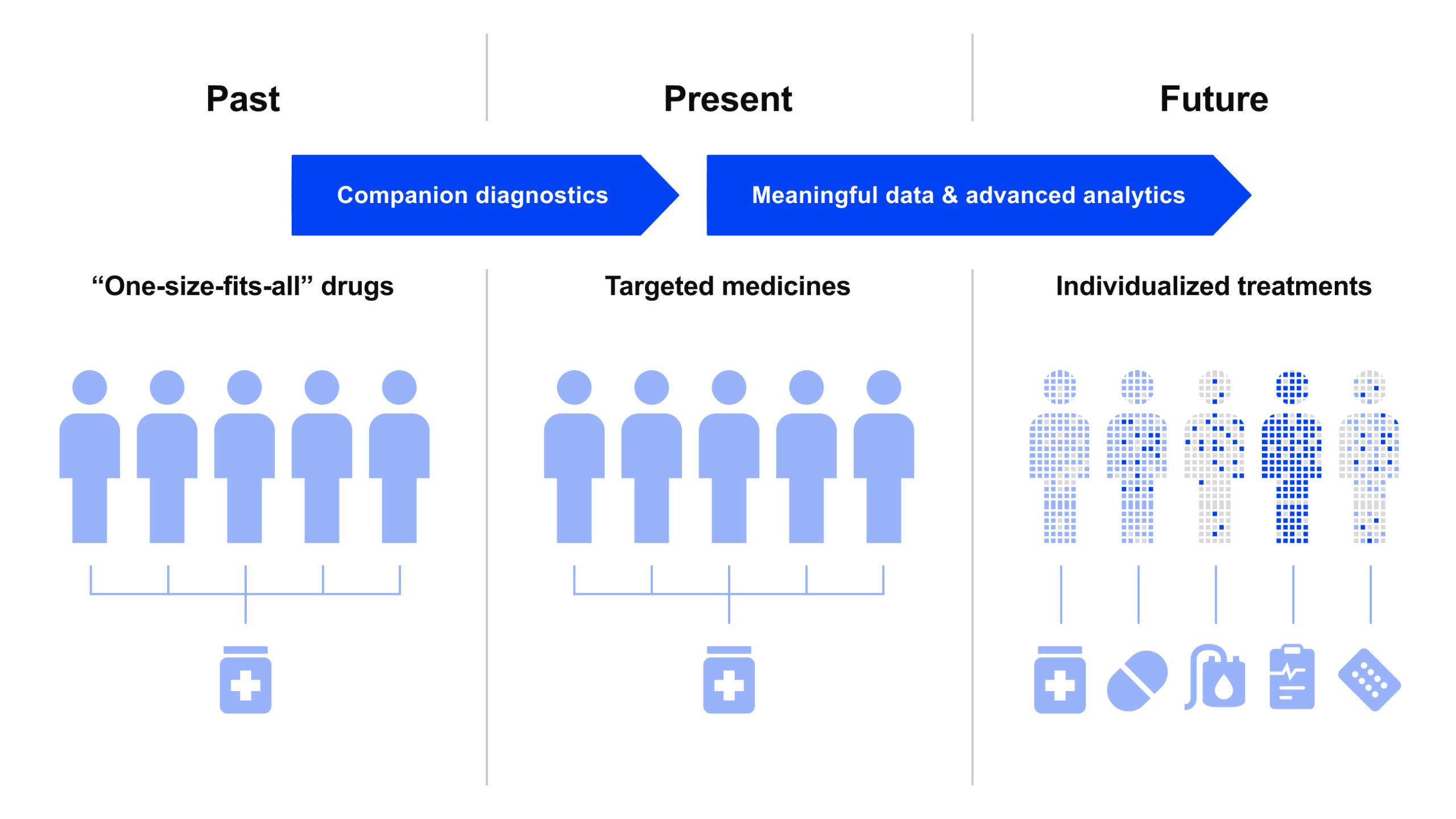
In practice, this could mean adjusting clinical guidelines to fit the patient. For example, if general guidelines recommend screening for a condition at age 50, a personalized plan might start earlier for a patient with a strong family history of that condition. Treatment decisions, follow-up intervals, and preventive measures are all customized.
In many European countries, insurance companies try to encourage patients to undergo preventive check-ups by reimbursing part of the cost. However, a systemic limitation remains: if a check-up is not formally indicated by standard clinical protocols—even if a patient’s personal risk factors clearly suggest it is needed—the insurer will typically refuse reimbursement. Personalized care exposes this gap between standardized rules and individual patient needs, highlighting why guideline adjustments are necessary for better outcomes.
This often requires clinicians to deviate from universal checklists and use their judgment in the context of the patient’s health data and preferences. While standard clinical guidelines remain a vital foundation, they may need adjustments in timing or intensity for certain patients to maximize benefit. Such individualization can significantly improve clinical outcomes and patient experience, as care is more relevant to each person’s needs.
The benefits of moving to personalized healthcare are compelling. Studies show that personalization can improve clinical outcomes and reduce healthcare costs in the long run. By detecting illnesses early and focusing on prevention, patients are less likely to require expensive, invasive treatments down the road. For instance, catching and managing a chronic condition in its early stages can avoid hospitalizations or complications later, saving both lives and resources. Personalized care also tends to foster a deeper patient-provider connection, as patients feel heard and understood when their care aligns with their individual story. This experience of tailored care often leads to higher patient satisfaction and engagement in their own health.
Why Pursue Personalized Care? Challenges and Long-Term Payoffs
The case for personalized care is clear—better outcomes, higher patient satisfaction, and potentially lower costs—but implementing it is not without challenges. In the short term, personalizing care can seem more resource-intensive. It may require more diagnostics (like genetic tests or specialized screenings) and longer clinician-patient interactions to gather information and counsel patients.
These investments, however, pay off in the long term by lowering costs associated with advanced disease treatment and by improving efficiency. Research indicates that personalized healthcare reduces treatment costs and leads to favorable long-term clinical outcomes. In other words, spending effort and resources now to tailor prevention and therapy can avert far more expensive problems later, such as emergency surgeries or unmanaged chronic illnesses.
Time concerns are a major barrier. Clinicians today are extraordinarily busy, often burdened by documentation and administrative tasks. A study found that for every hour doctors spend face-to-face with patients, they spend nearly two additional hours on electronic records and desk work. In a typical 15-minute appointment, there is scant time to delve into a patient’s full background, risk factors, and lifestyle—topics essential for personalization.
Many routine visits focus narrowly on immediate issues and test results, leaving limited opportunity to discuss prevention or long-term health planning. Thus, even if a provider wants to personalize care, the current healthcare workflow doesn’t easily allow it. This time crunch contributes to clinician burnout and means critical insights about the patient might be missed.
Another challenge is scale and resources. Personalized care tends to be easier in theory for a small practice or a city district clinic, where providers know their community well. In reality, however, even at a local level, delivering tailored care to every individual can overwhelm available resources.
For example, a pilot program in a small town might successfully personalize care for its residents, but it often relies on extra staff time, community health workers, or specialized support that may not be sustainable without significant investment. When expanding such efforts to larger populations, the need for management of huge amounts of data and coordination rises exponentially.
This leads back to the initial problem: more personalized attention per patient requires more time and more resources per patient, which health systems struggle to provide under current constraints.
So how can healthcare organizations implement personalized care without breaking the bank or overburdening clinicians? The key is to work smarter, not harder, and this is where automation and smart use of data come in.
By leveraging modern health IT tools, we can cheaply scale personalized care. In the next sections, we explore how technological solutions, especially FHIR for healthcare transformation efforts and AI, can help bridge the gap. The right tools can ensure that personalized care is not only feasible, but efficient, making it possible to implement even at the level of small communities or clinics and then scale up.
Ultimately, investing in personalization is a classic case of short-term effort for long-term gain. The challenge is getting through that transition period by using innovations that lighten the load on human providers while maintaining a high standard of care.
Automation and Data: Enabling Personalized Healthcare at Scale
To overcome the challenges above, healthcare needs to embrace technology that can automate routine work and seamlessly connect data from many sources. The vision is to have a 360-degree view of each patient—their medical history, genomics, wearables data, lifestyle metrics—without adding extra burdens on clinicians. Two innovations are pivotal in this regard: standardized data exchange via HL7 FHIR, and AI-based automation. Together, these technologies form the backbone of a smarter, more efficient healthcare architecture that supports personalization.
Data Interoperability with HL7 FHIR
Any discussion of healthcare data today inevitably leads to interoperability: the ability of systems and devices to exchange and understand data. HL7 FHIR has emerged as the leading standard to achieve this. FHIR defines a common format for health data and a set of APIs, so information from disparate systems can be shared and aggregated easily. In fact, regulators are pushing for its adoption: the U.S. Centers for Medicare & Medicaid Services (CMS) issued an interoperability rule that essentially mandates using standards like FHIR for smoother data exchange between patients, providers, and payers.
Compliance with such regulations means hospitals and clinics must structure and open up their data in standardized ways—a foundational step toward personalized care, since an individual’s data often resides in many silos (primary care, specialists, hospitals, fitness apps, etc.).
FHIR has been around for some time; it’s built for the modern web era, making data sharing more like exchanging information on the internet rather than parsing old-school documents. By using FHIR, a patient’s electronic health record data, lab results, medication lists, and even device readings can all be encoded in a consistent format. This interoperability means a clinician (or an algorithm) can retrieve a comprehensive patient profile on demand, combining information that was once fragmented across different systems.
For healthcare organizations, implementing FHIR may involve upgrading legacy systems or adding a translation layer. Some opt for an FHIR “facade” essentially a wrapper that sits on top of older databases and outputs data in FHIR format. (This approach lets organizations participate in FHIR-based data exchange without a complete backend overhaul—see our blog on FHIR facade pros and cons for more details.) The bottom line is that personalized healthcare with FHIR data is far more achievable when all relevant information can flow into one unified view.
Crucially, FHIR’s design also accommodates new data sources that are increasingly important for personalization. Wearable fitness trackers, smartwatches, blood pressure cuffs, glucometers, and other patient-generated data can be incorporated via FHIR interfaces. Imagine a clinician or care platform having a single, lifelong record of all care provided to an individual, from birth to the present, including data from personal devices like smartwatches and health apps.
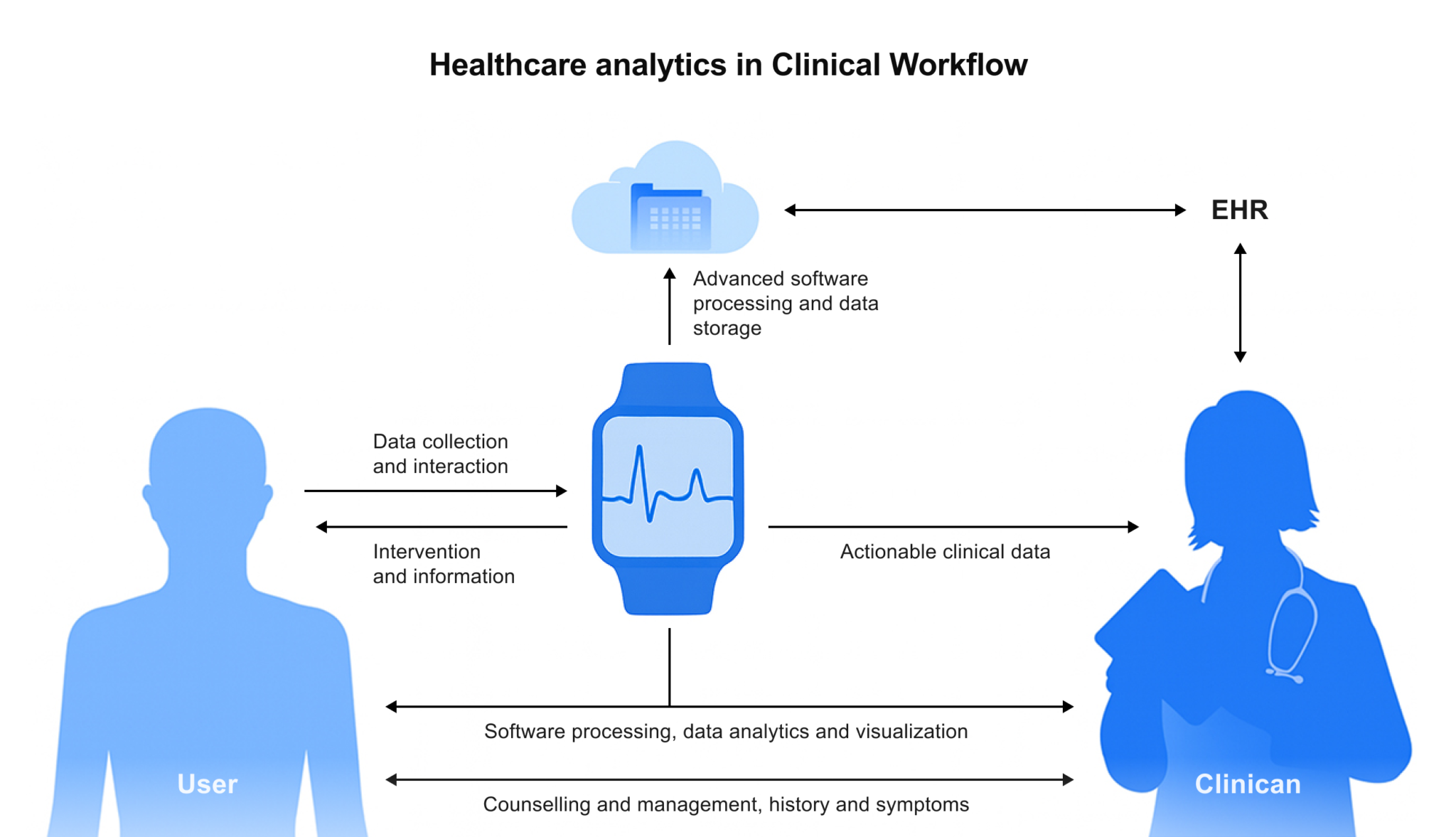
Not only providers, but patients and insurers would benefit from this personalized healthcare with FHIR integration, as it offers a single source of truth for informed decision-making.
“A single, lifetime view of health data that merges clinical and personal sources would lead to better diagnoses, safer emergency care, improved follow-ups, and appropriate long-term management.”
In essence, FHIR enables that “single source of truth” by standardizing how diverse systems communicate. Health IT teams can use an enterprise-grade solution like a FHIR server (for example, Edenlab’s Kodjin platform) as the platform to store and exchange this data, ensuring the infrastructure is robust enough to handle large volumes and secure by design. With the right FHIR-based architecture in place, any authorized application—whether a doctor’s EHR interface or a patient’s mobile app—can access the data it needs, when it needs it.
AI and Automation in Clinical Workflows
Collecting and standardizing data is only half the battle; making sense of it and reducing manual workload is the other half. This is where AI, especially machine learning and intelligence automation, comes into play. Modern AI tools can act as an extra pair of hands (and eyes and ears) for the healthcare team, handling repetitive tasks and analyzing complex data patterns. By using FHIR to improve patient engagement and data accessibility, AI systems can quickly tap into a patient’s interoperable record and perform functions that save clinicians time and support personalized decisions.
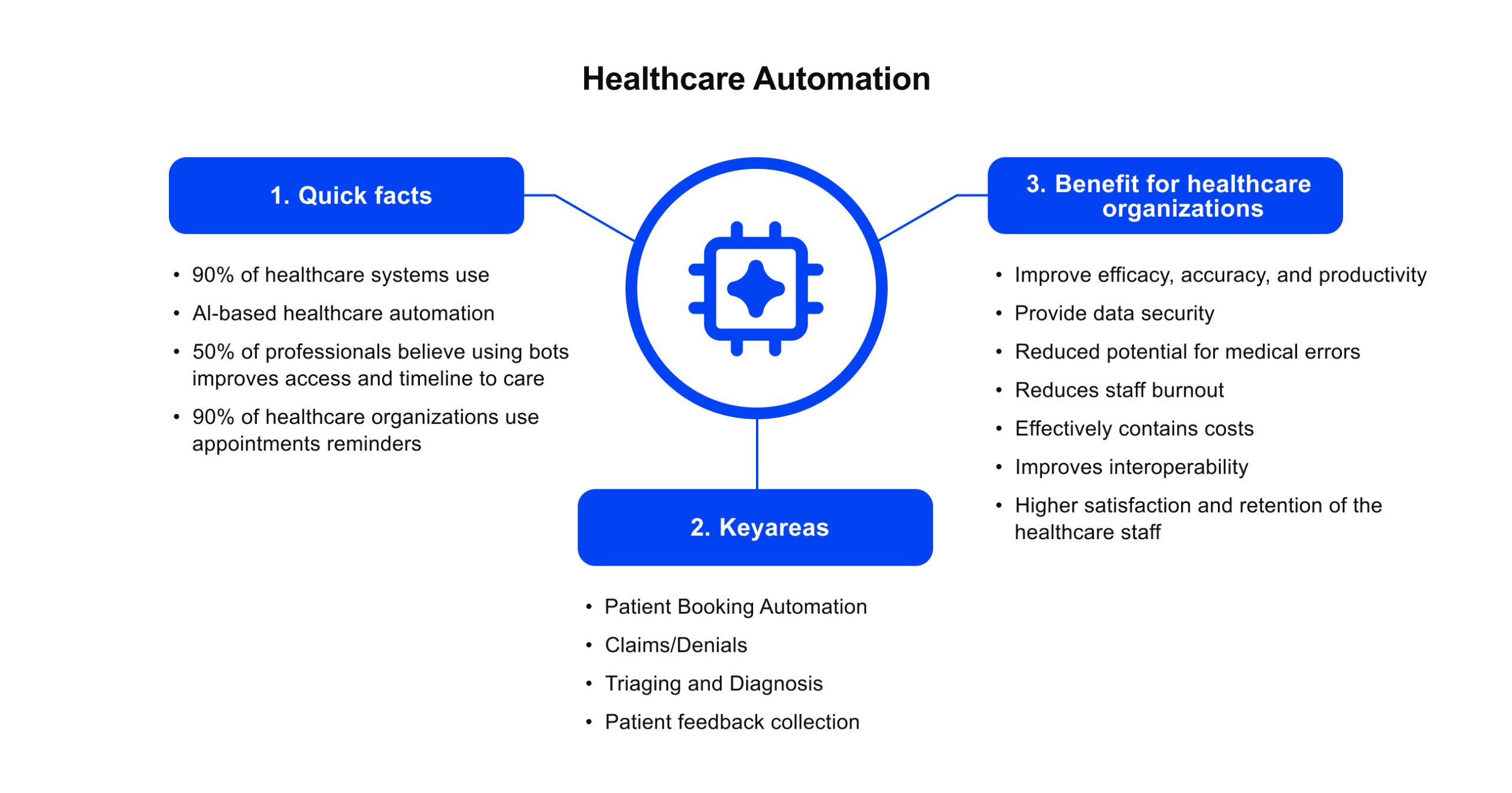
One immediate impact of AI is automating routine administrative and documentation tasks. For instance, AI-powered medical scribe technology can listen to a patient visit (or parse a recording) and automatically generate visit notes, fill out forms, and even highlight key details, all of which get stored in the EHR without the clinician typing them.
By taking over burdensome data entry, AI gives providers precious time back to spend with their patients. As Harvard Medical School experts note, AI can automate tasks to free up clinicians’ time to focus more on face-to-face patient care, reducing the cognitive burden and helping prevent burnout.
Doctors can also use AI to quickly summarize a patient’s past history or pull out relevant trends from the chart, which supports better decision-making. In a sense, agentic AI systems for healthcare can gather information from various data streams and present insights so that the human provider can make the final call.
The result is that the clinician is liberated from many menial tasks and can concentrate on the complex, human-centric aspects of care that truly require their expertise. This shift doesn’t just benefit doctors; patients ultimately get more attention and a more personalized interaction rather than watching their caregiver spend the visit typing on a computer.
AI is also proving invaluable in clinical decision support, which is central to personalized medicine with FHIR data as fuel. With comprehensive, standardized patient data available, machine learning models can analyze an individual’s information against vast datasets to generate tailored risk predictions and treatment suggestions.
For example, AI algorithms can scan a patient’s combined data (genetics, labs, symptoms, etc.) and help identify which treatment is likely to be most effective for that specific person. Today, AI can help clinicians better personalize treatment regimens by finding patterns in similar cases and predicting who will respond best to certain interventions.
This is the promise of precision medicine coming to life, using data-driven insights to choose the right drug or therapy for the right patient at the right time. Such AI-driven guidance can complement clinical intuition and ensure no relevant detail (no matter how small or buried in the record) is overlooked when formulating a care plan.
Another area where AI shines is remote monitoring and early warning systems, which directly support personalized, proactive care. Because FHIR allows data from wearables and home-health devices to flow into the medical record in real time, AI can continuously analyze this data for any signs of trouble.
From automating paperwork to synthesizing complex data for clinical insights, AI’s contributions ultimately circle back to one thing: letting humans do what they do best. By handling the heavy data lifting and monotonous chores, AI lets clinicians spend more time listening, empathizing, and thinking critically about each patient’s care.
It also empowers patients: for instance, through AI-driven apps or chatbots that can give personalized coaching or answer questions using a patient’s own data, thereby using FHIR to improve patient engagement outside clinic walls. When mundane tasks are automated and data is organized, the healthcare experience becomes more human for everyone involved. Doctors and nurses can be fully present with patients, and patients feel like active partners in a health journey tailored for them.
Reduce documentation burden and operational friction with AI solutions designed for regulated healthcare environments.
We are here to help. Check our
Healthcare AI solution developmentFHIR + AI: A Path to Truly Personalized Care
Individually, both HL7 FHIR and AI are powerful tools, but together they form a synergy that addresses the core challenges of personalized healthcare. Personalized healthcare with FHIR integration ensures that all relevant patient information is accessible and shareable, breaking down data silos. Meanwhile, AI acts on that rich data, finding patterns and making routine processes more efficient.
This combination directly tackles the earlier challenges we discussed: it mitigates the time burden on clinicians, helps manage long-term costs through preventive focus, and makes it feasible to implement personalization even in resource-constrained settings by amplifying the impact of each provider.
Consider how these pieces fit together in a real-world care setting. A patient’s data from various clinics, hospitals, and personal devices converge via FHIR into a single view. An AI-powered system continuously monitors this data, alerting the care team to any red flags (for example, a drop in lung function for an asthma patient or an irregular heart rhythm detected by a smartwatch).
At a routine appointment, the physician doesn’t start from scratch or sift through paper records; instead, they see a synthesized dashboard of the patient’s health trends, risk scores, and care gaps generated by AI from all that interoperable data. The physician can then focus on the patient, discussing personalized strategies, perhaps adjusting a medication dose based on genetic markers, or scheduling a screening test earlier than guidelines suggest because the patient’s profile indicates higher risk.
Throughout this process, the patient is also engaged via digital tools: they might have an app (powered by the same data and AI) that educates them about their conditions and reminds them of individualized preventive actions. In short, the ecosystem of personalized healthcare with FHIR data plus AI ensures everyone – providers and patients alike – has the information they need, when they need it, to make informed health decisions.
Implementing this vision does require investment and coordination, but it’s becoming more accessible. Healthcare IT companies are forging partnerships to deliver end-to-end solutions that marry interoperability and intelligence.
Conclusion
Personalized healthcare is no longer a distant ideal; it’s within reach, thanks to the convergence of interoperability and artificial intelligence. By structuring data with FHIR and applying AI-driven automation, healthcare providers can finally deliver care that treats you as you, not as an average patient on a chart.
The journey comes with challenges in the short term, from adapting workflows to ensuring data privacy and management, but the long-term rewards are immense: healthier populations, more efficient use of resources, and a healthcare system that learns and improves with every individual it serves.
Using FHIR to personalize healthcare data and automating what can be automated allows doctors and nurses to regain time and insight, so they can practice the art of medicine at the top of their game. The result is a transformation of patient care, one where high-tech and high-touch go hand in hand.
With HL7 FHIR enabling seamless data exchange and AI turning data into actionable knowledge, the vision of truly personalized medicine is becoming a reality. It’s an exciting time for healthcare, as we stand on the cusp of delivering the right care for the right person at the right time, consistently and at scale. In other words, FHIR and AI just might lead to healthcare transformation and make personalized healthcare the new normal in the years ahead.

We dive deep where others skim
Tell us what data sources you have, what outcomes you want to improve, and where clinicians lose time today. We will propose a practical FHIR + AI roadmap.
FAQs
Is implementing FHIR difficult for healthcare organizations with existing legacy systems?
Implementing FHIR is not inherently difficult, but the challenge depends on how old and fragmented the existing systems are. Most healthcare organizations avoid heavy migrations by using an FHIR facade, which translates legacy data formats into FHIR without replacing core systems. This makes adoption significantly easier and faster.
What is the typical timeline for implementing a personalized healthcare solution using FHIR, and what are the key phases involved?
A typical personalized healthcare project built on FHIR takes about three to nine months. It usually starts with assessing current systems and designing the architecture, then moves into mapping existing data to FHIR, developing integrations and APIs, testing interoperability and security, and finally, going live with optimization and user onboarding.
What level of internal IT resources is required to maintain and manage FHIR-based personalized healthcare solutions after implementation? Does Edenlab offer ongoing support and maintenance?
After deployment, maintaining an FHIR-based solution doesn’t require a large internal team. One to three IT engineers can usually handle routine monitoring and minor updates. Edenlab covers the rest, offering ongoing support, SLA-based maintenance, scaling, upgrades, security updates, and help with new integrations.
How can Edenlab help implement FHIR in my healthcare system?
Edenlab assists with every stage of FHIR implementation: assessing your current environment, designing the interoperability strategy, deploying the Kodjin FHIR Server, modeling and mapping your data, building the necessary APIs, integrating EHRs, mobile apps, wearables, and national registries, and ensuring the solution stays reliable and compliant long-term.
Stay in touch
Subscribe to get insights from FHIR experts, new case studies, articles and announcements
Great!
Our team we’ll be glad to share our expertise with you via email










