FHIR-based claims auto-adjudication engine
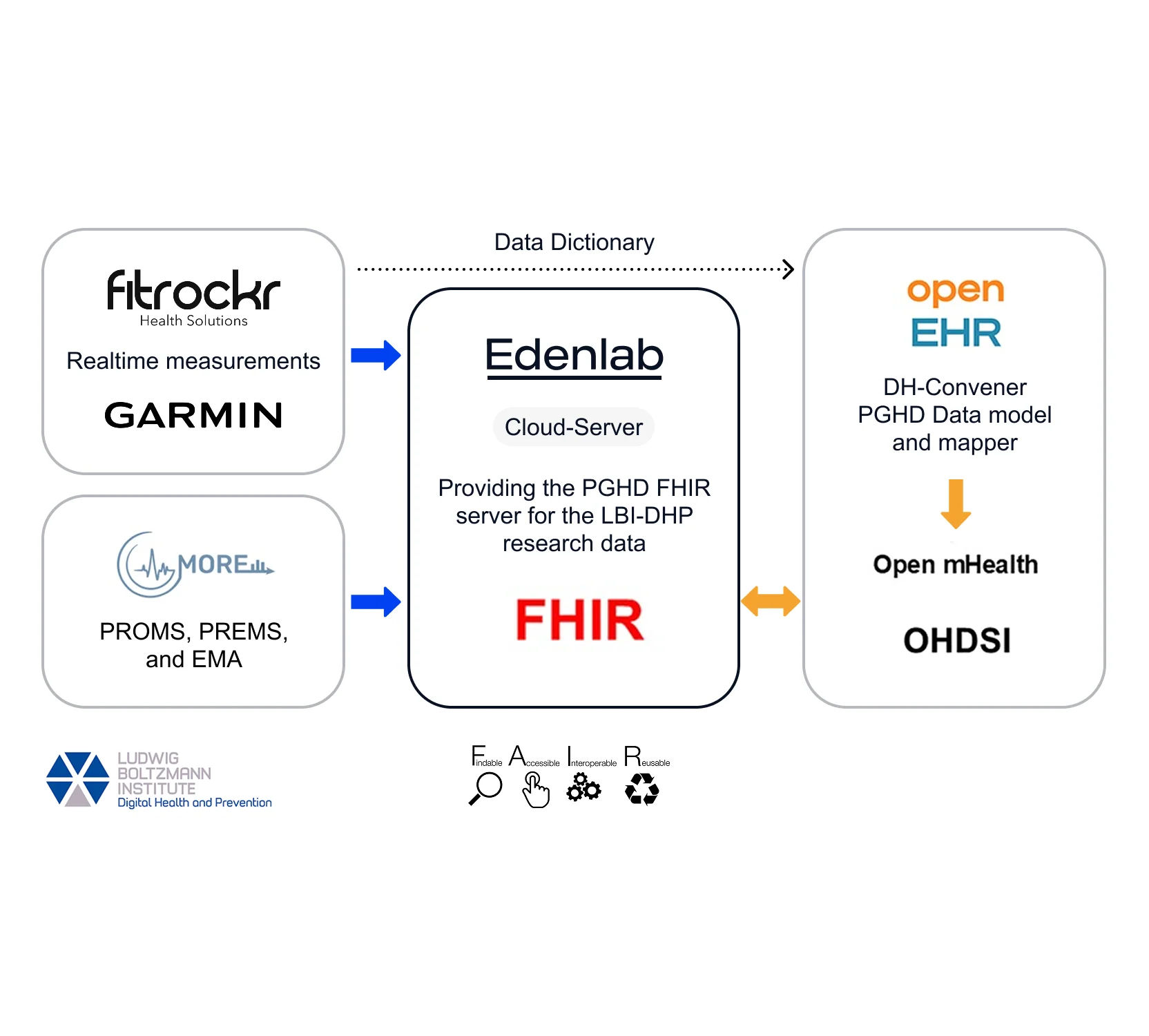
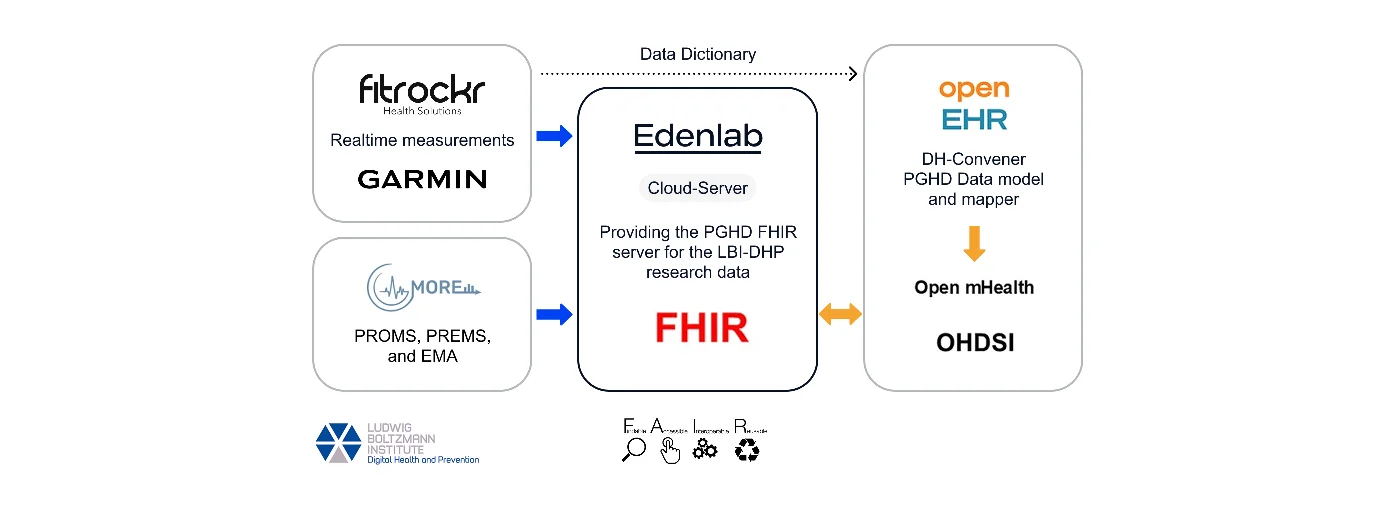
An auto-adjudication healthcare engine was one of the projects Edenlab developed for Heals.Asia, one of the largest TPAs in Hong Kong. Heals.Asia provides operational services, such as claims processing for all the major health insurance companies in Hong Kong, and exchanges data with the key health providers in the region.
As one would expect for a TPA (or any other administration or operational services company), greater efficiency and cost reduction are crucial for the business. Claims adjudication automation can obviously help with that, but it’s easier said than done. The main workload of TPAs is carried by the adjusters, who should have vast expertise and deep knowledge of the logic, rules, constraints, etc. of the services they are responsible for administering. One complication is that such logic, rules, and constraints (which constitute the insurance plans) are usually stored as non-structured, non-formalized, and fragmented data. The same applies to patients’ claim histories from various providers.
Therefore, in order to unlock the automation part of auto-adjudication, the Edenlab team first needed to resolve two quite complex issues:
– unification of the data exchange from different providers and insurers, and
– formalization and structuring of the insurance plans so Heals.Asia could support digital claim adjudication systems later.
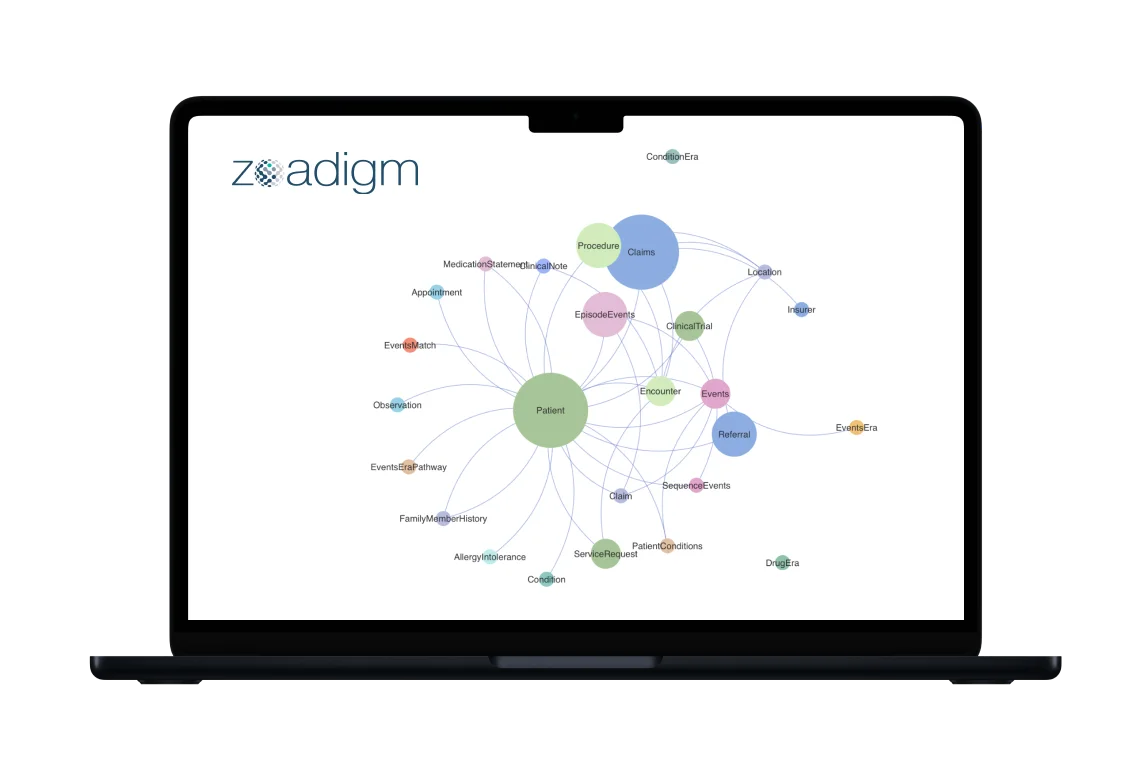
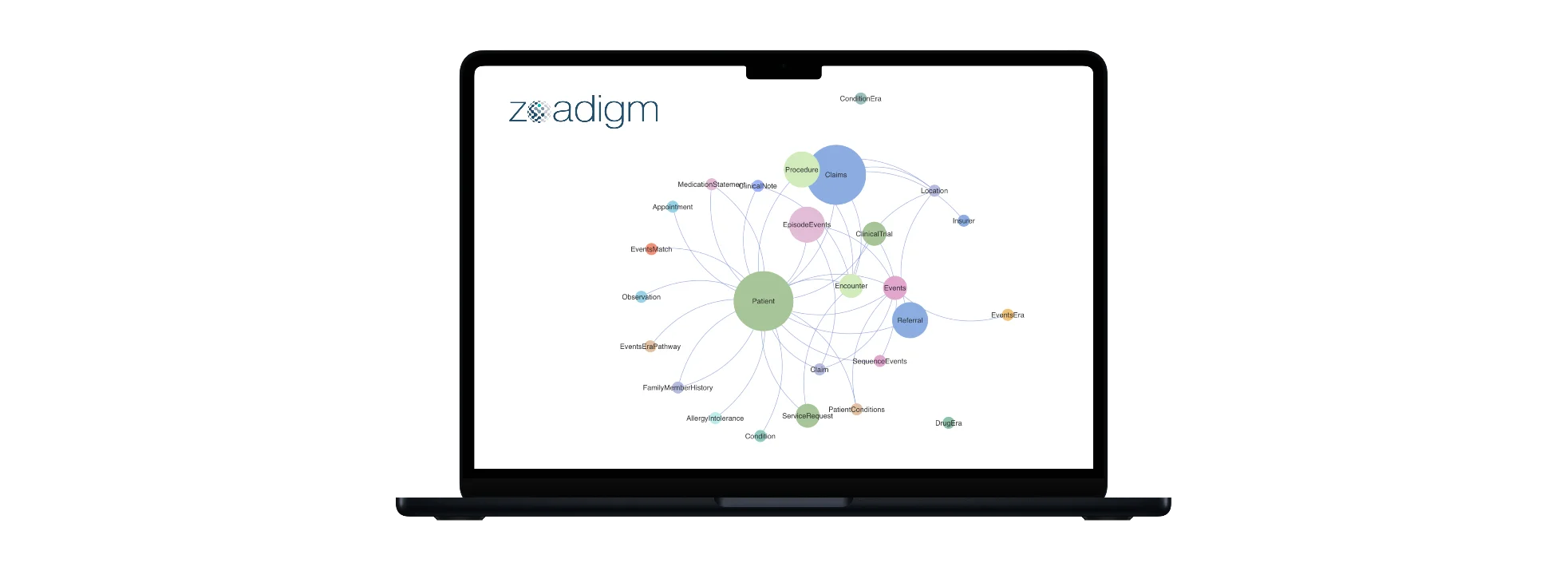
The first one was solved by mapping custom data structures to FHIR standards and by development of custom profiles for Coverage, CoverageEligibilityRequest, CoverageEligibilityResponse, Claim (for claims, predetermination, and pre-authorization), ClaimResponse, etc.
The second one was the starting point in the development of the auto-adjudicated claims engine this case study is dedicated to.